Slow It Down! A Mindful Yoga Practice for Pelvic Floor Health and Beyond

“Ok, let’s try that again, but I want you to do it a little bit more slowly.”
“Let’s see if you can do that with a little bit less tension.”
“Do you feel how your neck is working while you’re trying to move your hips? Let’s see if you can do that with only moving your hips.”
These are statements (or variations of them) that I tend to make most days of the week. One of the most common things I notice in the men and women I treat with persistent pelvic pain is difficulty in modulating tension. I generally can see this from the moment they walk in my office:
-
Gripping postures, sitting with the shoulders elevated, gripping the chest or the glutes, tightening the back
-
Minimal variability of movement, meaning it is difficult for them to move in different patterns, fully bend and rotate their spines and hips, etc.
-
Altered breathing patterns with poor diaphragmatic excursion
This type of high-tension behavior often occurs in conjunction with a dominant sympathetic nervous system. In these cases, the body feels continuously threatened, which makes sense if you’ve had pain for a long time and don’t seem to get better.
This can lead to the “fight-or-flight” response being pushed into overdrive. When this occurs, we typically see amped-up muscle tension, changes in breathing patterns, and many additional physiological compensations.
I believe this pattern tends to also lead to an overly gripped, hypervigilant pelvic floor muscle group. Then, what I typically see is that instead of the pelvic floor activating with variability, based on the required task at hand (meaning, small amounts of activation for small tasks, and large amounts of activation for bigger tasks), I see loss of force modulation with very high amounts of activation for basic tasks, and an inability to let go of that force for simple tasks or tasks that require relaxation (bowel movements, sex, etc).
Slowing It Down 
So, with all of that being said, one of the best things a person with persistent pelvic pain can do is to learn to slow down and control his or her tension patterns. My patients typically begin working on this within the first week or so of treatment, and we continue working on this throughout the initial phase of their care.
Our goal is to create awareness of movement—to move mindfully and truly feel what the body is doing to accomplish a task.
Typically, as a person becomes more mindful of the movements he or she is performing, we will see an alteration in the force required to perform the movement. This, along with other treatments we are working on, encourages a shift of the body from an overly sympathetic state to a more neutral one.
So, how can you get started with slow and mindful movements if you are struggling with persistent pelvic pain?
First, if you are already working with a pelvic physical therapist (PT), talk with them about your tension strategies. Ask her if she has noticed you moving with higher tension and discuss integrating slow and mindful movements within your treatment program. If you are not in pelvic physical therapy or wish to try something on your own, here is one of my favorite exercises to start with:
The Pelvic Clock Exercise
-
This exercise is adapted from a Feldenkrais movement (I believe). I love it because I can integrate diaphragmatic breathing with pelvic floor relaxation, and it encourages awareness of the movement of the pelvis. I tend to find that many people with pelvic pain have difficulty truly knowing where their pelvis is in space and how it moves, and this exercise can help to improve that. So, let’s get started.
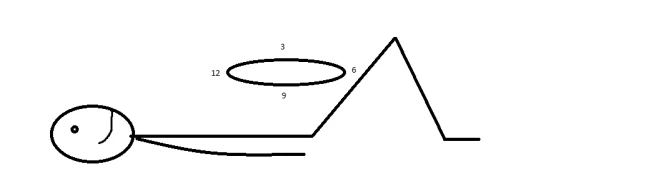
-
Begin in a relaxed, comfortable position, lying on your back on a mat with your knees bent and your feet resting on the mat (bed, floor, whatevs). Visualize a clock sitting on your pelvis, as is shown in the picture above.
-
Start with slow, diaphragmatic breathing. Remember, breathing with your diaphragm will allow the ribcage to expand in all directions. The belly and chest will lift, but the muscles of your neck and shoulders should stay relaxed. If you have not read much about diaphragmatic breathing, read this post.
-
Next, we will start to integrate your pelvic floor into your breathing. So, on the next inhalation, visualize the breath allowing your pelvic floor to lengthen and relax. This should not be something forceful (i.e., don’t push out your pelvic floor), but rather, just focus on letting go of tension as you inhale, allowing the pelvic floor and abdominal wall to gently lengthen to let go of any tension.
-
Next, we will add in the gentle movement of the pelvis with your breath. As you inhale, the pelvic floor will relax, and the pelvis will gently tilt toward 6 o’clock (allowing the tailbone to fall toward the mat). As you exhale, gently tilt the pelvis back to 12 o’clock, allowing the low back to slowly come into contact with the mat. Repeat this slow pattern, focusing on trying to use small amounts of muscle tension to accomplish the task. Remember that this movement, and any other movement, should not cause you to guard, tense your muscles, or drive up any of the pain you are experiencing.
-
Once you feel confident and comfortable with the previous step, you can begin to add the rotational component. This time, as you inhale, slowly rotate the pelvis around the clock shifting from 12 –> 3 –> 6, ending in the position where your tailbone is gently dropped toward the mat. As you exhale, allow the pelvis to rotate from 6–> 9–> 12, ending in the position where your low back is gently resting on the mat. Repeat this pattern for several breaths, then try to reverse the motion (inhaling as you move from 12 –>9–>6 and exhaling from 6–>3–>12).
-
Challenge yourself further by trying to allow the pelvis to move through all the numbers of the clock (12–>1–>2–>3… etc).
Remember, there is no rush to performing this exercise! The purpose is awareness—to really feel your pelvis move and to shut off any additional tension in performing the task.
Did you feel your neck tighten as you were moving? Try again with a focus on keeping it relaxed.
Are your legs tightening and moving frequently as you move through the clock? Try to see if you can calm that tension and isolate the movement to your pelvis.
Do you feel your pelvic floor gripping as you move? Try to see if you can keep the emphasis on relaxing the pelvic floor during your breathing.
Why Practice Slow Yoga? 
The pelvic clock can be practiced on its own or as a warmup for a mindful yoga asana practice. Slowing down your yoga practice can both calm your nervous system and give you the opportunity to pay closer attention to the process of unfolding in each asana.
Yoga poses are, after all, a process. They are not stone statues that we attain and then hold. They are living, breathing entities. Try slowing down and using the ideas from the pelvic clock practice—especially awareness of pelvic floor movement—in all the asanas you practice. Then take time between each pose to feel the residue.
Don't Miss this Exciting New Course with Lynn Crimando: Yoga for Strength-Training: Keys to Building a Stronger Body-Mind with Yoga.
Reprinted with permission from Jessica Reale, PT.com
 Jessica Reale is a Doctor of Physical Therapy (DPT) and Board-Certified Specialist in Women’s Health (WCS) practicing in Atlanta, GA. She owns and treats patients at Southern Pelvic Health, a private practice serving men, women, and children with pelvic floor dysfunction in the metro Atlanta area. Jessica graduated from Duke University with a Doctor of Physical Therapy degree and Gordon College with a BS in Kinesiology.
Jessica Reale is a Doctor of Physical Therapy (DPT) and Board-Certified Specialist in Women’s Health (WCS) practicing in Atlanta, GA. She owns and treats patients at Southern Pelvic Health, a private practice serving men, women, and children with pelvic floor dysfunction in the metro Atlanta area. Jessica graduated from Duke University with a Doctor of Physical Therapy degree and Gordon College with a BS in Kinesiology.
She loves working with all people who have pelvic health problems– this includes urinary, bowel, and/or sexual dysfunction, as well as pelvic pain. She confesses to spending way too much time reading new articles to try to integrate the most current research and practices into treatment plans. Jessica also works with children who have constipation, bladder difficulties or bedwetting, or persistent abdominal pain.




